In the intricate realm of human anatomy, there exists a subtle yet immensely significant network of muscles and tissues that often remains shrouded in mystery—the pelvic floor. While it may not be a topic that readily springs to mind in everyday conversation, the pelvic floor plays a pivotal role in our daily lives, affecting not only our physical well-being but also our overall quality of life. Welcome to the world of pelvic floor dysfunction—a captivating and enigmatic facet of our bodies that holds secrets you never knew you needed to unravel.
In this blog, we will embark on a journey to explore the depths of this fascinating subject, diving deep into the nuances of its function, the challenges it presents, and the strategies to maintain a harmonious pelvic floor. Prepare to be intrigued and enlightened as we unveil the mysteries of this vital but often overlooked aspect of human health.
It is often disheartening to see narratives of individuals of the male gender who have actively sought medical assistance but have encountered insurmountable barriers in accessing appropriate healthcare. When a patient experiences pain, discomfort, and a decline in physiological function, they may find it profoundly discouraging to get a diagnosis from their physician indicating the absence of any underlying medical condition. When these individuals find themselves in the presence of their healthcare provider or primary care physician, they often experience feelings of desperation and depression.
The science and research on pelvic floor dysfunction
One study claims that chronic pelvic pain syndrome (CPPS), another name for pelvic floor dysfunction, is one of the most misdiagnosed and undertreated illnesses affecting men’s health. This research reveals a global incidence rate of up to 16% among men, making it the most prevalent urologic condition among males under the age of 50. According to the Prostatitis Foundation, it is estimated that around half of the male population may have prostatitis over their lifetime.
“Symptoms can be present on average for 87 months before diagnosis” is the number that most disturb me. According to Smith (2016), the duration of 87 months corresponds to a period exceeding 7 years, during which an individual endures a state of distress prior to obtaining a diagnosis for their condition. It is hardly surprising that these individuals are experiencing a sense of desperation.
What exactly is pelvic floor dysfunction?
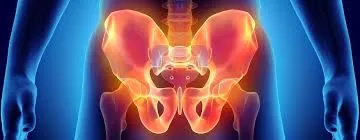
Pelvic floor dysfunction refers to a condition characterized by the impaired functioning of the pelvic floor muscles, ligaments, and connective tissues, which form a supportive hammock-like structure at the base of the pelvis. These muscles and tissues play a crucial role in supporting and controlling various pelvic organs, including the bladder, uterus, and rectum. When the pelvic floor muscles do not function properly, it can lead to a range of distressing symptoms and complications.
This problem can manifest in different ways, including urinary incontinence (the involuntary leakage of urine), fecal incontinence (involuntary bowel movements), pelvic organ prolapse (the descent of pelvic organs into the vaginal canal), chronic pelvic pain, and sexual dysfunction. This condition can affect individuals of all ages and genders, although it is more prevalent in women, especially after childbirth and during menopause. The causes of pelvic floor dysfunction are multifaceted, including factors such as pregnancy, childbirth trauma, obesity, chronic constipation, aging, and connective tissue disorders.
Diagnosis typically involves a thorough medical history and physical examination and may include specialized tests such as urodynamic studies or pelvic floor muscle assessments. Management of pelvic floor dysfunction often includes a combination of lifestyle modifications, physical therapy, behavioral strategies, and, in some cases, surgical interventions. Effective treatment aims to reduce symptoms, enhance pelvic floor muscle coordination and strength, and improve the overall quality of life for those who suffer from this condition, which we will look into in detail.
Are pelvic floor dysfunction and prostatitis the same?
No, pelvic floor dysfunction and prostatitis are not the same conditions; they are distinct medical issues that affect different parts of the body and have different causes and symptoms.
Prostatitis:
- Prostatitis is an inflammatory condition that affects the prostate gland, which is a male reproductive organ located just below the bladder. There are different types of prostatitis, including acute bacterial prostatitis, chronic bacterial prostatitis, chronic prostatitis/chronic pelvic pain syndrome (CP/CPPS), and asymptomatic inflammatory prostatitis.
- Although non-bacterial prostatitis (such as CP/CPPS) may not have a clear infectious cause, bacterial infections are frequently the cause. during urination or ejaculation, and flu-like symptoms in some cases.
- Although non-bacterial prostatitis (such as CP/CPPS) may not have a clear infectious cause, bacterial infections are frequently the cause.
- Diagnosis involves a medical history, physical examination, and often laboratory tests, including urine and prostate fluid cultures.
- Treatment depends on the type and cause of prostatitis and may include antibiotics for bacterial infections, pain management, and lifestyle changes.
Pelvic Floor Dysfunction:
- Pelvic floor dysfunction refers to problems related to the muscles, ligaments, and connective tissues that support the pelvic organs, including the bladder, uterus, and rectum. These issues can lead to symptoms such as urinary incontinence, fecal incontinence, pelvic organ prolapse, chronic pelvic pain, and sexual dysfunction.
- Pelvic floor dysfunction can affect both men and women, although it is more commonly associated with women, particularly after childbirth or during menopause.
- It may result from various factors, including pregnancy, childbirth trauma, obesity, chronic constipation, aging, and connective tissue disorders.
- Diagnosis involves a physical examination and specialized tests, and treatment often includes lifestyle modifications, physical therapy, behavioral strategies, and, in some cases, surgical interventions.
We have discussed that both these dysfunctions are two distinct medical conditions with different causes, symptoms, and areas of the body they affect. Pelvic floor dysfunction involves issues with the pelvic floor muscles and support structures and can affect both men and women, whereas prostatitis is an inflammatory condition of the prostate gland and is specific to men. It is important to consult with a healthcare provider for proper diagnosis and treatment of these conditions if you experience related symptoms.
Chances of the wrong diagnosis
Pelvic floor dysfunction may be wrongly identified and diagnosed as “prostatitis.” This word encompasses a wide range of symptoms, serving as a comprehensive categorization. Prostatitis, in its true form, refers to a bacterial illness that specifically affects the prostate gland. Based on the aforementioned research, it is evident that less than 10% of the cases may be classified as genuine instances of prostatitis. The diagnosis is often modified to “chronic prostatitis” or, alternatively, “non-bacterial chronic prostatitis.”
I would like to clarify that I am not expressing any kind of criticism against medical professionals. Upon inquiry, the majority of physicians expressed unfamiliarity with the aforementioned disease. Additionally, they noted that this subject is not often addressed during medical education. Given the limited coverage of this issue in medical school curricula, it falls upon specialists to disseminate knowledge and raise awareness, enabling men to get the appropriate assistance they need.

General questions Discussed While determining this Issue?
The array of symptoms is extensive and perplexing. Individuals with chronic pelvic pain syndrome may exhibit a wide range of symptoms, which may vary significantly from one man to another. The following is a compilation of inquiries that a medical professional might pose to individuals of this nature:
- The occurrence of pain in the penis, particularly at the tip, shaft, urethra, and scrotum, subsequent to sexual activity and ejaculation is being discussed.
- Do reductions in size, increased rigidity, decreased sensation, poorer erectile responses, and erectile dysfunction accompany the phenomenon of penile retraction?
- Experiencing discomfort in the perineum (also known as the taint), bladder region, below the belt buckle, lower back, groin, and hips?
- Are there any instances of diminished feeling, diminished orgasm, or diminished ejaculation present in your condition?
- Do you have symptoms such as urinary urgency, increased frequency of urination, painful urination, intermittent flow, a thin or weak stream, or dribbling?
- The individual may have symptoms such as constipation, diarrhea, inadequate voiding, frequent voiding, and increased difficulty maintaining cleanliness.
- Which factors have a greater impact on one’s well-being: laying, sitting, standing, time of day, physical exercise, or stress?
Treatment for pelvic floor dysfunction
Treatment and precautions for pelvic floor dysfunction of the condition. Here are some general guidelines for managing pelvic floor dysfunction:
- Lifestyle Modifications:
- Maintain a healthy weight. Excess weight can put additional strain on the pelvic floor muscles. Losing weight through a balanced diet and regular exercise can help alleviate some symptoms.
- Manage constipation: Chronic constipation can strain the pelvic floor muscles. Ensure you have a high-fiber diet, drink plenty of water, and establish regular bowel habits to prevent constipation.
- Pelvic Floor Muscle Exercises (Kegel Exercises):
- Pelvic floor physical therapy is often a primary treatment approach. A physical therapist can teach you how to perform Kegel exercises correctly to strengthen and improve the coordination of your pelvic floor muscles.
- Kegel exercises can help with urinary incontinence, fecal incontinence, and pelvic organ prolapse.
- Behavioral Strategies:
- Bladder and bowel training: Developing a regular schedule for urination and bowel movements can help reduce urgency and leakage.
- Biofeedback: Biofeedback therapy can provide visual or auditory cues to help you better control your pelvic floor muscles.
- Medications:
- To maintain posture symptoms, your healthcare provider may prescribe medications such as anticholinergic drugs for over-periods, adders, or laxatives for constipation.
- SurgStayical Interventions:
- In some cases, surgical procedures may be recommended to correct severe pelvic organ prolapse or other structural issues. These surgeries are typically considered after conservative treatments have been ineffective.
Precautions for managing pelvic floor dysfunction
- Avoid high-impact exercises: Activities like heavy lifting, high-impact aerobics, and exercises that strain the pelvic floor, such as certain yoga poses, should be approached with caution. Consult with a physical therapist or healthcare provider for guidance on safe exercise options.
- Maintain good posture: Proper posture can help alleviate pressure on the pelvic floor. Avoid sitting or standing for extended periods, and practice good body mechanics when lifting heavy objects.
- Stay hydrated: Drinking enough water is essential for overall health, but excessive fluid intake, especially caffeine and alcohol, can irritate the bladder. Balance your fluid intake to avoid overloading your bladder.
- Dietary modifications: Some foods and drinks, like spicy foods, citrus fruits, caffeine, and alcohol, can irritate the bladder and exacerbate urinary symptoms. Consider keeping a food diary to identify and limit triggers.
- Manage stress: Stress and anxiety can exacerbate pelvic floor dysfunction symptoms. Stress-reduction techniques like meditation, deep breathing exercises, and yoga may help manage symptoms.
- Pelvic floor health during pregnancy and postpartum:
- Pelvic floor dysfunction is common during and after pregnancy. Consult with a healthcare provider or pelvic health specialist for guidance on exercises and techniques to support pelvic floor health during this time.
You should not be shy about consulting a specialist if conservative treatments do not yield significant improvements. Consider consulting with a urogynecologist, urologist, or pelvic floor physical therapist who specializes in pelvic floor dysfunction.
It’s essential to work closely with your healthcare provider to develop a personalized treatment plan tailored to your specific symptoms and needs. Pelvic floor dysfunction is a manageable condition, and with the right interventions and precautions, you can significantly improve your quality of life.
Disclaimer:
The author’s views are his or her own. The facts and opinions in the article have been taken from various articles and commentaries available in the online media, and Eastside Writers does not take any responsibility or obligation for them.
Note: Contact our Writers at www.eastsidewriters.com for writing Blogs/Articles on any niche. We have experts in various domains from Technology to Finance and from Spirituality to Lifestyle and Entertainment.






